Neuromodulation of sacral roots
When should neuromodulation be considered?
Sacral root neuromodulation is an innovative technique used to treat certain urinary or pelvic disorders that are resistant to conventional treatments. It regulates the nerve activity responsible for controlling the bladder, rectum and perineum.
Neuromodulation can be proposed in the following situations:
✔ Overactive bladder (urgent urges, leakage, frequent urination),
✔ Functional urinary retention (inability to urinate without a mechanical cause),
✔ Chronic pelvic pain or painful bladder syndrome,
✔ Some cases of severe constipation or anal incontinence , after multidisciplinary consultation.
It is indicated when first-line treatments (medication, perineal rehabilitation, botulinum toxin injections) are ineffective or poorly tolerated.
Origin of the disorders concerned
Neuromodulation addresses functional pathologies, where the dysfunction lies in the communication between the brain, the spinal cord and the pelvic organs.
These disorders can be linked to :
- underlying neurological pathology (multiple sclerosis, spinal cord injury, spina bifida),
- or be idiopathic (with no known cause) but resistant to conventional treatments.

Treatment objective
The goal of neuromodulation is to “retrain” the nervous system by gently stimulating the sacral nerve roots (primarily S3) with low-frequency electrical impulses. This technique allows for: • reduce overactive bladder, • restore a normal sensation of urinary urge • improve or trigger bladder emptying, • relieve chronic pelvic pain.Treatment sequence
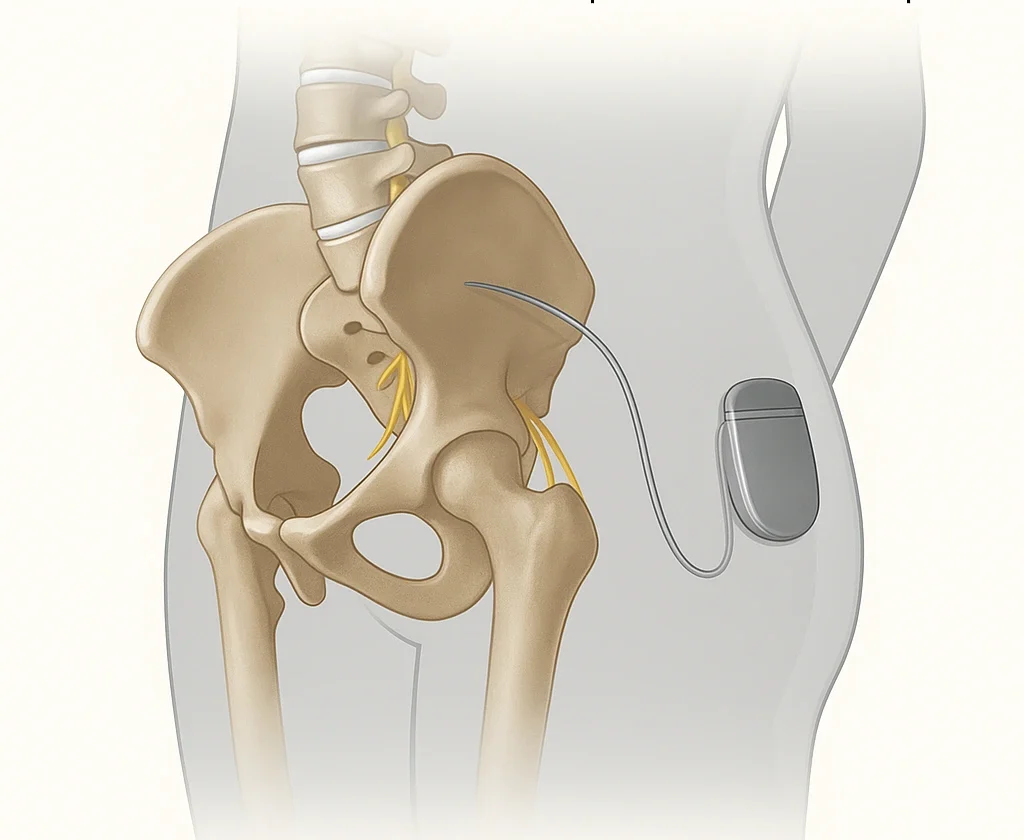
Step 1: Testing phase (or evaluation phase) • Performed on an outpatient basis, under local or light anesthesia. • Implantation of a thin electrode near the sacral root (often S3). • Connection to an external neurostimulator for 1 to 3 weeks. • Objective: to evaluate the effectiveness on urinary and pelvic symptoms. • The patient keeps a voiding diary to note improvements. If the test phase shows an improvement ≥ 50%, the final implantation is carried out. Step 2: Neurostimulator Implantation • Performed under light general anesthesia. • The stimulator (the size of a USB key) is implanted under the skin, at the top of the buttock. • Permanent connection to the test phase electrode. • Programmable and adjustable device available for consultation.Post-operative follow-up
– Program and adjust the stimulator as required. – Regular follow-up by Dr Laurence Peyrat and/or a specialist nurse. – Replace the housing every 5 to 10 years, depending on the model used.Expected results
– High success rate: improvement in 70-80% of selected cases. – Long-lasting, well-tolerated effects. – Significant improvement in quality of life, especially for patients with complex or resistant urinary disorders.Possible side effects
• Transient pain at the implantation site, • Electrode displacement (rare), • Discomfort related to the case (especially for thin people), • Need for adjustment or reprogramming in case of loss of efficiency. Stimulation can be stopped at any time, without permanent consequences.Why consult Dr Laurence Peyrat?
✔ Latest-generation neuromodulation techniques.
✔ Personalized support throughout the entire process (testing phase, implementation, follow-up).
✔ Possible collaboration with neurologists, gastroenterologists, pain centers.
✔ Specialist in functional and pelvic urology, with recognized expertise in the management of complex voiding disorders.
My video review
Let me introduce you to the principle of sacral neuromodulation. It is a minimally invasive treatment that gently stimulates the sacral nerves to improve urinary control and relieve chronic pelvic disorders .
A first step towards an effective solution
Make an appointment today to benefit from attentive listening and support tailored to your situation.
